Editor’s Note: I know you’re up to your neck in alligators and may not have time to read this entire article. If that’s the way it is, please do the right thing and click here to add your input to the most important freediving research ever.
The human body has been studied inside and out since the beginning of, well, human bodies and few who read these lines lack appreciation of the the medical arts, or of progress in the related sciences and technologies. If we know of an event, a structure, process or state in the body of a living human being, more than likely we can measure it with terrific precision and even see it – often in real time and non-invasively. Be that as it may, when Kirk Krack launched his career as a freediving pioneer , he quickly found out that pioneers don’t get a lot of help from road maps or signs.
Uh, that’s how come they’re pioneers. The same medical and scientific culture which could nonchalantly replace the heart of a living person had precious little to say about apnea diving. Much of the conventional medical wisdom could be summarized thus: No, you can’t do that. It’s impossible. It is beyond the capabilities of the human body.
But… we were doing it, and had been doing it.
As Kirk’s infant Performance Freediving initiative developed he made heavy and ongoing investments in science, which in the context of a struggling and often impoverished enterprise was nothing less than visionary. It takes a lot of belief and no small courage for a struggling entrepreneur (a guy living on students’ and colleagues’ sofas) to sink time and money into projects which have no immediate prospect of an economic payoff. Kirk’s own curiosity, the same unquenchable thirst for exploration and adventure which took him from the Saskatchewan prairie to a global oceaneering career, was certainly one motivator but more importantly, Krack understood that there’s a deep symbiosis between freediving’s vitality as a recreational and competitive sport, on the one hand, and the empty shelf he’d discovered in the great Library of Science.
Freediving needed science, and science needed freediving. Both are in the business of boldly going where no-one has gone before, and there sure is where to go.
A number of physicians and scientists have, over the years, passed through the Performance Freediving world as clinic students, each adding new knowledge to Kirk’s growing database but also taking away observations that have fueled new research and analysis.
An early partnership struck with Simon Frasier University in Vancouver,BC, continues with a regular program of activities, measurements, analysis and reporting. So, too, it’s no coincidence that the Performance Freediving Team’s newest member is a physician and an inventor of medical devices. Dr. George ‘Doc’ Lopez, 58, is a US National record holder in the Free Immersion discipline and Founder/CEO of ICU Medical Devices, a global leader in safey medical systems. Doc Lopez is a walking ( and freediving) example of the synergistic effects of practical experience and a scientific background.
More recently a distinguished pulmonologist from the Cedars-Sinai Medical Center in Los Angeles, Dr. Ralph Potkin, has been organizing an ambitious program of freediving-related research. Dr. Potkin is no neophyte to dive medicine. He’s been an active scuba diver since 1971 and has dived all over the world – including Antarctica, for all you been-there-done-that braggarts. He’s made hyperbaric medicine his primary specialty for the past ten years and has founded the Beverly Hills Center for Hyperbaric Medicine. Potkin, an alumnus of the Performance Freediving clinics, resided with the team during the train-up for the Sink Faze Cayman 2006 World Record event and recorded pre- and post-dive physiologicals from team and support freedivers.

Dr. Potkin’s scientific interest in freediving has roots in his earlier study of decompression sickness in marine mammals. The finding that whales, seals and dolphins can indeed suffer DCS prompted him to wonder about the vulnerabilities of human freedivers. His current work is in the nature of a pilot study, the intent of which is to develop a basis for a formal research program. Read on – there’s a role for you in this project.
Ralph Potkin wants to explore three basic research issues, the first of which is whether, indeed, the phenomena associated with DCS can be observed in freedivers.
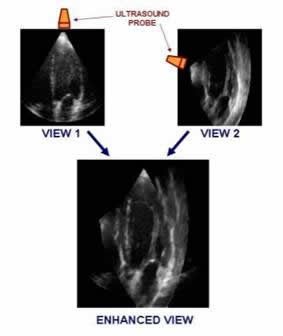
The measurement technologies are well-developed and have served the field of scuba diving, buthad never been applied to systematic data collection in freediving. The basic tool here is Doppler bubble detection. A small, rugged device non-invasively detects bubbles in the blood vessels as the nitrogen dissolved in tissues under hydrostatic pressure (at depth) expands under ambient surface air pressure.
Ancillary questions address the frequency with which significant nitrogen absorption occurs during freediving, the depth, time and other factors associated with incidence, and, as a practical matter, mitigation. When and how are freedivers at risk for DCS, and what can we do to prevent it?
Dr. Potkin recently disclosed that he’s found bubble formation in some freedivers examined shortly after diving. He’s understandably reluctant to be more specific at this early juncture, but it’s fair to say that his findings on Grand Cayman and elsewhere favor moving forward with the research.
A second broad area of research underway centers on the issue of long-term neurological effects of freediving. This is, of course, a hot-button item with the general public and more than a few freedivers themselves. Who hasn’t had a non-diving friend or relative declare that holding one’s breath deprives the brain of oxygen and leads to certain neurological damage? So? Is it true? Are we dumbing ourselves down?
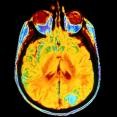
It’s one of those things that ‘everybody knows’, but which turns out to be not exactly so.
The evidence for the protective effects of the mammalian dive reflex under apnea – diversion of blood to the most vital organs, bradycardia and so forth – is strong and is, as Dr.Potkin reminds us, surprising to the conventional medical wisdom. Having learned of a theretofore unknown homeostatic mechanism which seems to allow for some degree of apnea without harmful consequence, Dr. Potkin argues for asking the question at the margins. It may be that a seemingly innocuous activity, one ‘provided for’ by human physiological response, has consequences which become apparent only over time. Or, it may be that there are immediate limits to the adaptation afforded by the diver reflex: limitations of depth, time, frequency, other factors or combinations of factors.
Dr. Potkin is addressing the neurological issue with a preliminary program of brain imaging, focused on subjects who have a lengthy history of deep freediving. I’ve been a subject in these imaging studies, and it is an astounding and more than a bit disconcerting thing to see one’s own thinkum-dinkum at work in high–res. I guess mine still works to some degree – there were significant changes in my brain activity following a very annoying session of computerized cognitive puzzle-solving.
The phenomenon we colloquially term ‘squeeze’ is the third major area Dr.Potkin is interested in, with etiology (i.e., causes) and prophylaxis (prevention) as his immediate medical concerns. He is, after all, a chest doctor. He’s taken spirometry data from the Performance Freediving team members and support freedivers during the Sink Faze trainup and collected anecdotal data from as many freedivers as he could. Here, too, it is premature to report anything in the nature of a finding. There is this, though: Dr. Potkin has observed very significant increases in lung volume after what we call ‘packing’. Common knowledge, you say ? Duh ? Not so – Dr. Potkin assures us that the medical community would poppycock the notion that human lung volume can be increased from a non-pathological baseline by any known intervention. You do it, but just so you know: it can’t be done.
I did it in June, 2006 at Cedars-Sinai Medical Center in Los Angeles. Surrounded by Dr. Potkin, some skeptical colleagues and technicians, and a few gazillion dollars’ worth of state-of-the-art high-res full-motion imaging gizmos, I have watched my own heart pumping blood: valves opening and closing, blood flowing through the chambers just like in the textbooks. I filled my lungs, stuffed 35 packs into ‘em, and watched the doctors’ numb fascination as my right heart chambers were squeezed flat, blood backwashing toward the lungs, and my blood pressure dropped in seconds to undetectable. All this sitting upright, fully conscious.
If only I had one of those gizmos at home ! Ralph is in the know, but his colleagues were shocked by what they witnessed. One told me that under normal circumstances, the images he saw and the vital signs readouts accompanying them would have thrown the hospital into a full-out emergency response.
The medical community has been surprised by previously unknown adaptive responses in human apnea divers, homeostatic programming which enables us to dive far deeper and longer than traditionally thought possible.
Dr. Potkin points out another thing that surprises the academics – the common knowledge ( in the freediving community) that the dive reflex is conditioned. Learned, and teach-able, too. Kirk Krack, for example, has shown ( over more than 1,000 clinic students) that ‘naïve’ (i.e., completely inexperienced) students can quickly be trained to accomplish breath-holds that only a few years ago were the province of the sport’s elite.
The possibility that many, or most human beings have much more extensive apnea capabilities than previously thought – much better, in a sense, than are neccesary – goes back to the tantalizing Aquatic Ape Hypothesis. The threads are woven together.
Dr. Potkin’s three research areas address issues of considerable practical concern for freedivers. DCS used to be thought of as an issue for scuba divers, but Dr. Potkin’s Doppler measurements have made it clear that there is a real, though as yet unquantified exposure for apnea divers as well. As performance parameters increase and more freedivers dive deeper and longer this issue will very likely become of greater concern to more people.
Nor can one regard the prospect of neurological damage with equanimity – we need to know more, and the sooner the better.
Finally, chest squeeze is a problem which has put a goodly number of our friends and colleagues out of the freediving business temporarily or, in some cases, permanently. Dr. Potkin sees the state of our knowledge in this area as primitive. He concedes there is no decisive evidence for the origin of the blood components seen in freedivers’ sputum from time to time. What, exactly is it, where is it coming from and why? If there are ways to prevent or mitigate this class of barotrauma, it were better we knew and practiced them
Since the Potkin research has direct and immediate consequences for the survival, health and well-being of all freedivers, it seems to me we should be willing to share our experience and knowledge with the investigator. What we have is folklore – there’s a lot of good knowledge there, as the doctors acknowledge – but it’s not systematized and doubtless includes some bogus theorems and superstitions. We can teach science things it never knew about the human body, things that may well have prophylactic and even therapeutic implications way beyond the freediving scene. Science, in return, can help us put our knowledge in order, guiding us to safer practices and better performance.
There’s a way you can join in this effort and make a significant, immediate contribution. No, don’t grab you wallet, it’s not money that’s needed from you – it’s your experience and knowledge. Please take the time to visit the Potkin research website here.
The brain you pick may be your own.
